Carcinoid Syndrome Treatment
Home » For Patients old » Living with NETs » Carcinoid Syndrome » Carcinoid Syndrome Treatment
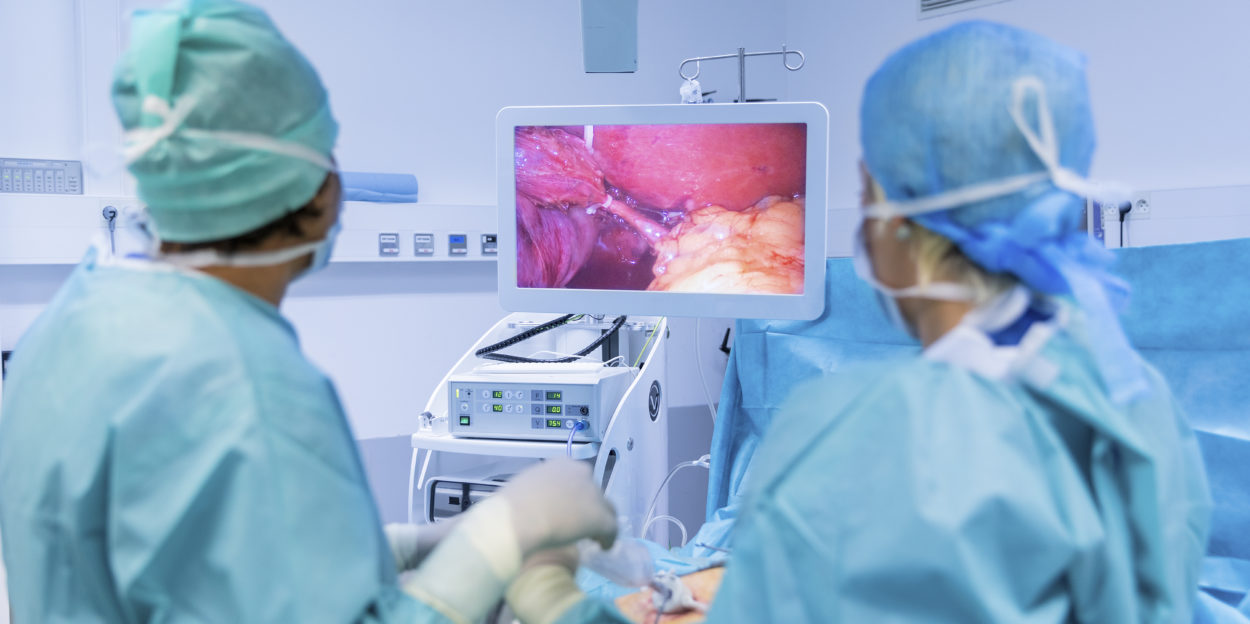
How is carcinoid syndrome treated?
There are a variety of carcinoid syndrome treatments, including somatostatin analogs and other medications, liver-directed therapies, surgery, and chemotherapy.
Medications for carcinoid syndrome treatment
Somatostatin analogs
Somatostatin is a naturally occurring hormone produced in the body. The function of somatostatin is to inhibit (reduce or limit) the release of gastrointestinal and endocrine hormones in the body, some of which are substances (e.g., serotonin) that contribute to carcinoid syndrome. A somatostatin analog is a medication that mimics the function of somatostatin and can reduce the production and release of substances by tumors that cause carcinoid syndrome.1 Somatostatin analogs include Octreotide and Lanreotide. 2,3
- Octreotide is available as a short-acting medication that is administered daily by injection just beneath the skin (subcutaneous injection). Octreotide is also available as a long-acting medication. The long-acting form of Octreotide is called Sandostatin LAR and can be administered monthly as an intramuscular injection.
- Lanreotide, also called Somatuline Depot, is another long-acting somatostatin analog that is also administered monthly.
Both Octreotide and Lanreotide have similar effectiveness and provide symptom relief in 50% to 70% of people with carcinoid syndrome.3 Additionally, multiple studies have indicated that both Octreotide and Lanreotide inhibit the growth of tumor cells.3
Common side effects include nausea, abdominal bloating, and fatty stools (steatorrhea). People taking these drugs may also experience gallstone formation and associated complications. Somatostatin, and thus somatostatin analogs, reduce the motility and contraction of the gallbladder which can occasionally cause gall-stone formation.3
Targeted therapy
Oral medications that act upon specific cell signaling pathways (such as mTOR, VEGF, VEGF-A) may be used in combination with other approaches to treat carcinoid syndrome.5
Telotristat
Telotristat is a recently approved drug that reduces the production of serotonin in the body. The drug is used in combination with a somatostatin analog to control diarrhea associated with carcinoid syndrome.2
Interferon
Interferons are substances that are produced naturally in the body. Interferon alfa may be used in combination with a somatostatin analog (e.g., Octreotide) to control symptoms of carcinoid syndrome that are difficult to or cannot be controlled with a somatostatin analog alone.2
Surgery for carcinoid syndrome treatment
Surgical treatments aim to remove or reduce the volume of NETs, causing carcinoid syndrome. Surgery is generally reserved for patients in which 90% of the tumor can be removed and who do not have compromised liver function or extensive liver metastases.2 The table below describes surgical treatments based on tumor type and location.
Summary of some surgical treatments by NET location and type3
Varied, Many tumors
Potential Surgical Options and Outcomes
Small Intestine
Liver
If liver metastases can be surgically removed, it often leads to the improvement of carcinoid syndrome symptoms.
Varied, many tumors
For patients with heavy tumor burden and metastases, tumor debulking (removing large portions of the tumor) may improve symptoms as well as extend and improve the overall health of the patient.
Lung/bronchial
If diagnosed early, bronchial NETs may be removed through surgery. The outcome of this therapy may offer total relief of symptoms caused by carcinoid syndrome.
Stomach and rectal
Surgical removal of stomach and rectal tumors (smaller than 1 cm) that are detected early may lead to total relief of the symptoms caused by carcinoid syndrome.
Read more about surgical treatments for NETs.
Liver-directed therapies for carcinoid syndrome treatment
Liver embolization therapy treats liver tumors by blocking the blood (or nutrient) supply to the tumor.5 By blocking the oxygen and nutrient supply, the tumor may be “starved” to death.
Embolization uses microparticles to block the blood supply to part or all the liver, depending on the extent of the disease.
- Chemoembolization combines liver embolization with chemotherapy.
- Radioembolization combines liver embolization and radiotherapy by coating microparticles for embolization with a radioactive compound called yttrium-90 (Y-90). The radiation is delivered to the tumor and can kill cancer cells.
- Radiofrequency ablation uses radio wave energy to deliver heat through a needle to cancer cells within the liver, thereby causing the cancer cells to die (ablation).
- Microwave ablation is similar to radiofrequency ablation but uses heat generated by microwave energy to kill the tumor cells in the liver.
Read further for additional information regarding liver-directed therapies for neuroendocrine cancer.
Chemotherapy for carcinoid syndrome treatment
Chemotherapy drugs aim to kill cancer cells and, in some cases, may shrink the tumor. Chemotherapy drugs are generally not helpful for quickly controlling the symptoms of carcinoid syndrome from well-differentiated NETs, and the use of chemotherapy is more commonly used in patients with higher grade and poorly differentiated NETs.
Read further for additional information regarding chemotherapy drugs, including other non-chemotherapy treatments that may be used for treating NETs.
Other therapy options for carcinoid syndrome treatment
Peptide Receptor Radionuclide Therapy (PRRT). PRRT is a nuclear medicine treatment that involves using a radioactive nuclide attached to a somatostatin analog. This systemic treatment delivers radiation directly to the tumor to kill cancer cells.

Xavier Keutgen, MD, University of Chicago
Surgery of NETs Watch Video
Michael Soulen, MD, University of Pennsylvania
Interventional Radiology Watch Video1 Ferrari A, Glasberg J, Riechelmann R. 2018. “Carcinoid syndrome: update on the pathophysiology and treatment.” Clinics (73) (supp 1): e490s.
2 Gade A, Olariu E, Douthit N. 2020. “Carcinoid syndrome: A review.” Cureus 12 (3): e7186.
3 Pandit S, Annamaraju P, Bhusal K. 2020. Carcinoid Syndrome. Internet: StatPearls. Accessed August 13, 2020. https://www.ncbi.nlm.nih.gov/books/NBK448096.
4 Oncolink. n.d. All About (Neuroendocrine) Carcinoid Tumors. Accessed August 12, 2020. https://www.oncolink.org/cancers/carcinoid-neuroendocrine-tumors/all-about-carcinoid-neuroendocrine-tumors.
5 Loughrey PB, Zhang D, Heaney AP. 2018. “New treatments for the carcinoid syndrome.” Endocrinol Metab Clin N Am 47: 557-576.
6 Howe J, Cardona K, Fraker D, et al. 2019. “The surgical management of small bowel neuroendocrine tumors consensus guidelines of the North American Neuroendocrine Tumor Society (NANETS).” Pancreas 46 (6): 715-731.
