Interventional Radiology as a Treatment for Neuroendocrine Tumors
Home » For Patients old » NET Tests & Treatments » NET Treatments » Interventional Radiology
Interventional radiology is a minimally invasive approach to treating neuroendocrine cancer that has spread to the liver. This approach starves liver tumors by denying them of the nutrients they need to grow and is often referred to as liver-directed therapy.
Hepatic Arterial Therapy
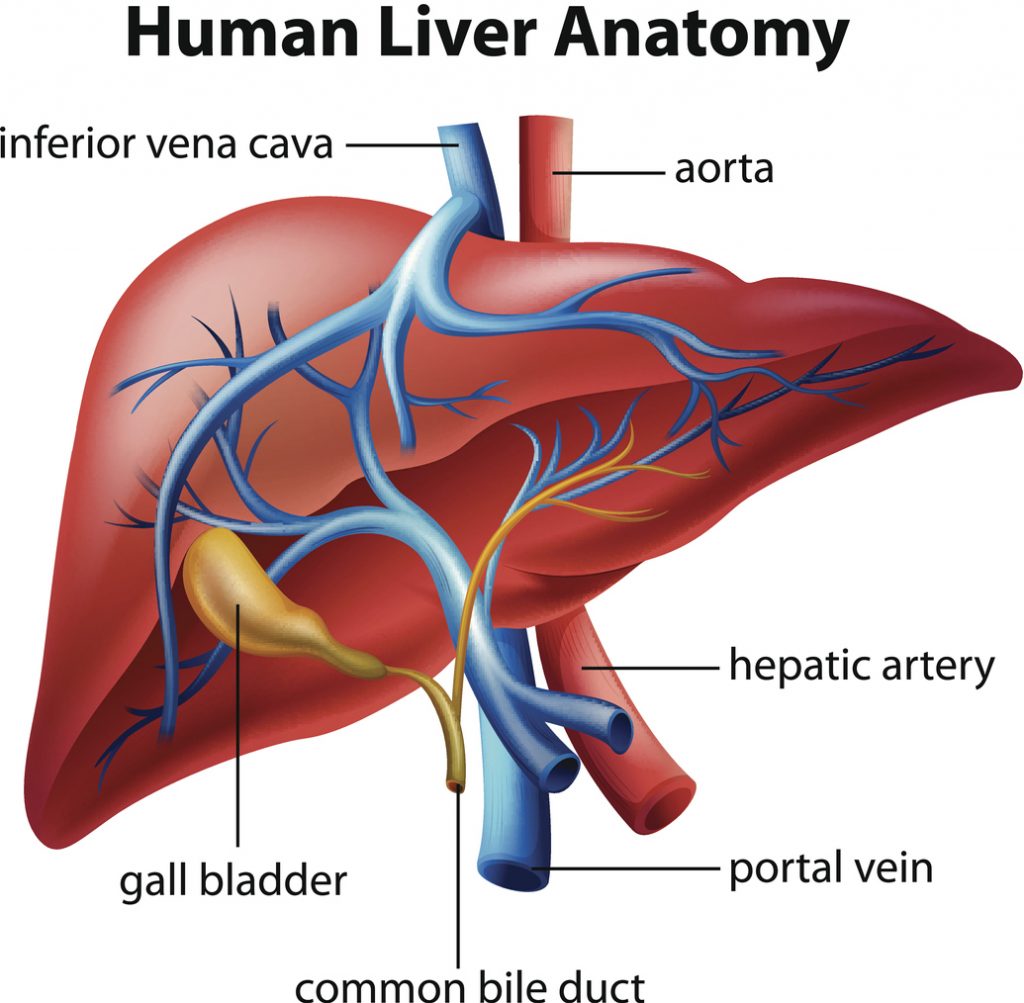
All cells require an adequate blood supply to survive. There are two sources of blood to the liver: the portal vein and hepatic artery.
- The portal vein mostly supplies blood to liver cells.
- The hepatic artery mostly supplies blood to liver tumors.
Hepatic arterial therapy reduces or blocks the flow of blood to stop cancer cells from getting the oxygen and nutrients they need to grow.
Hepatic embolization
A hepatic embolization blocks or reduces flow of blood in the hepatic vessel to kill cancer cells growing in the liver. The portal vein continues to supply blood to the liver. There are two types of hepatic embolization:
- Bland embolization: the injection of embolic particles, such as tiny gelatin sponges or beads (to reduce blood flow).
- Chemoembolization (TACE): the injection of embolic particles (to reduce blood flow) mixed with chemotherapy (to kill tumor cells) or direct injection of chemotherapy into the artery using a catheter.
Radioembolization combines embolization with radiation therapy to kill tumor cells in the liver. The doctor injects millions of radioactive microspheres (microscopic beads) into the hepatic artery, which emit radiation to kill tumor cells.
Radiofrequency Ablation (RFA)
Radiofrequency ablation (RFA) uses electrical current to destroy tumor cells. RFA involves placing a small probe into a tumor. This raises the temperature of the tumor tissue and destroys it. RFA can be done laparoscopically but is more commonly done in combination with liver resection.

Riad Salem, MD, Northwestern University
The latest in liver-directed therapies. Watch Video
Karen Grace, Northwestern University.
What is it like to undergo interventional radiology treatment? Watch Video
David Agarwal, MD, Indiana University.
Understanding interventional radiology Watch Video

