What is the difference between a pancreatic neuroendocrine tumor and a pancreatic tumor?
A few high profile celebrities, Aretha Franklin and Steve Jobs, have died from pancreatic neuroendocrine tumors. Following their deaths, their cancer was often called “pancreatic cancer” because it was cancer and it occurred in the pancreas. Why is this wrong?
Though they occur in the same organ, these are two different types of cancers. Pancreatic adenocarcinoma and neuroendocrine cancers have different:
- Causes
- Signs and symptoms
- Tests
- Treatments
- Outlooks
Pancreatic adenocarcinoma
Pancreatic adenocarcinoma is often referred to as “pancreatic cancer.” It starts in the exocrine cells, which produces enzymes to support digestion.
Pancreatic adenocarcinoma
- More common
- Poorer chance of recovery
- May not cause early symptoms. Advanced signs and late symptoms include:
- Jaundice (yellowing of the skin and whites of the eyes)
- Light-colored stools
- Dark urine
- Pain in the upper or middle abdomen and back
- Weight loss
- Loss of appetite
- Feeling very tired
Pancreatic neuroendocrine cancer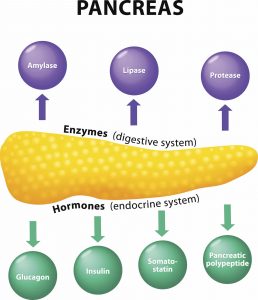
Pancreatic neuroendocrine cancer is sometimes called islet cell carcinoma. It starts in the endocrine cells, which produce hormones to regulate blood sugar.
Pancreatic neuroendocrine cancer
- Less common
- Better chance of recovery
- Tumors may produce hormones and cause early symptoms, such as:
- Diarrhea
- Indigestion
- Blood sugar changes
- Weight loss
- Stomach pain
- Jaundice (Yellowing of the skin and whites of the eyes)
- Skin rash on face, stomach, or legs
Where is the pancreas?
The pancreas is in the upper abdomen behind other organs such as the stomach, small intestine, liver, gallbladder, spleen, and bile ducts. It is about 6 inches long and shaped like a thin pear lying on its side.
What does the pancreas do?
The pancreas has two components:
- Exocrine pancreas produces enzymes that break down food in the small intestine
- Endocrine pancreas produces hormones that regulate blood sugar
Endocrine cells of the pancreas
The endocrine pancreas consists of endocrine cells that are arranged in “islets” and release hormones into the bloodstream. Neuroendocrine tumors arise from endocrine cells in the pancreas, which cluster together like an island and are called islet cells. These cells play an important role in regulating the body’s blood sugar.
One type of pancreatic neuroendocrine tumor, ιnsulιnoma, may lead to too much ιnsulιn and cause blurred vision, headache, fast heartbeat, and feeling lightheaded, tired, weak, shaky, nervous, irritable, sweaty, confused, or hungry.
Another type, called glucagonoma, can cause high blood sugar and cause headaches, frequent urination, dry skin, and mouth, or feeling hungry, thirsty, tired, or weak.
What is a neuroendocrine tumor?
Neuroendocrine tumors (NETs) are an uncommon cancer of the neuroendocrine cells, which receive messages from the nervous system and then release hormones into the bloodstream. When a neuroendocrine cell becomes cancerous, it divides uncontrollably, without stopping, forming tumors.
Primary sites for neuroendocrine tumors
NETs can occur throughout the body, but most commonly form in the:
- Gastrointestinal tract
- Pancreas
- Lungs
Since they arise in hormone-producing cells, a neuroendocrine tumor can overproduce hormones and release them into the bloodstream, causing a range of symptoms. These symptoms are commonly mistaken for other conditions such as irritable bowel syndrome, colitis, asthma, or menopause. One in two neuroendocrine tumor patients is misdiagnosed. On average, people have symptoms for five years before learning they have a neuroendocrine tumor. When it takes that long to obtain an accurate diagnosis, cancer can spread to other organs. More than half of NETs spread beyond the primary site before they are diagnosed.
Why does it matter? Raising awareness
Given delays in diagnosis, rates of metastases, and misdiagnosis, those affected by NETs advocate for increased education and awareness. Advocates for improvements in NET diagnosis and treatment stress the importance of referring to the cancer type, not site. No matter where it occurs, refer to this cancer as a neuroendocrine tumor to increase awareness for a misunderstood cancer.
Read more about pancreatic neuroendocrine tumors.
Browse NET patient videos on our YouTube channel.
Stay updated on neuroendocrine cancer. Subscribe to our newsletter.

NETWise Episode 1: What You Need to Know About NETs & NECs – Updated Episode
If you’re new to this show, welcome. You’re in the right place. Maybe you’ve been

Order Your Free Neuroendocrine Cancer Guide
Neuroendocrine Cancer: A Guide for Patients and Families Updated and expanded! Our easy-to-understand neuroendocrine cancer
Understanding Your Neuroendocrine Tumor Diagnosis
Understanding the grade and stage of neuroendocrine cancer and how that relates to prognosis.
